
Food insecurity, defined as difficulty in acquiring or accessing food due to a lack of money, affected one in nine of all U.S. households in 2018. Although trends in food insecurity are tracked through surveys of the general U.S. population, few surveys specifically focus on food insecurity among older adults. In December 2019 (prior to the COVID-19 pandemic), the University of Michigan National Poll on Healthy Aging surveyed a national sample of U.S. adults age 50–80 about household food insecurity and participation in food assistance programs.
Experiences with food insecurity
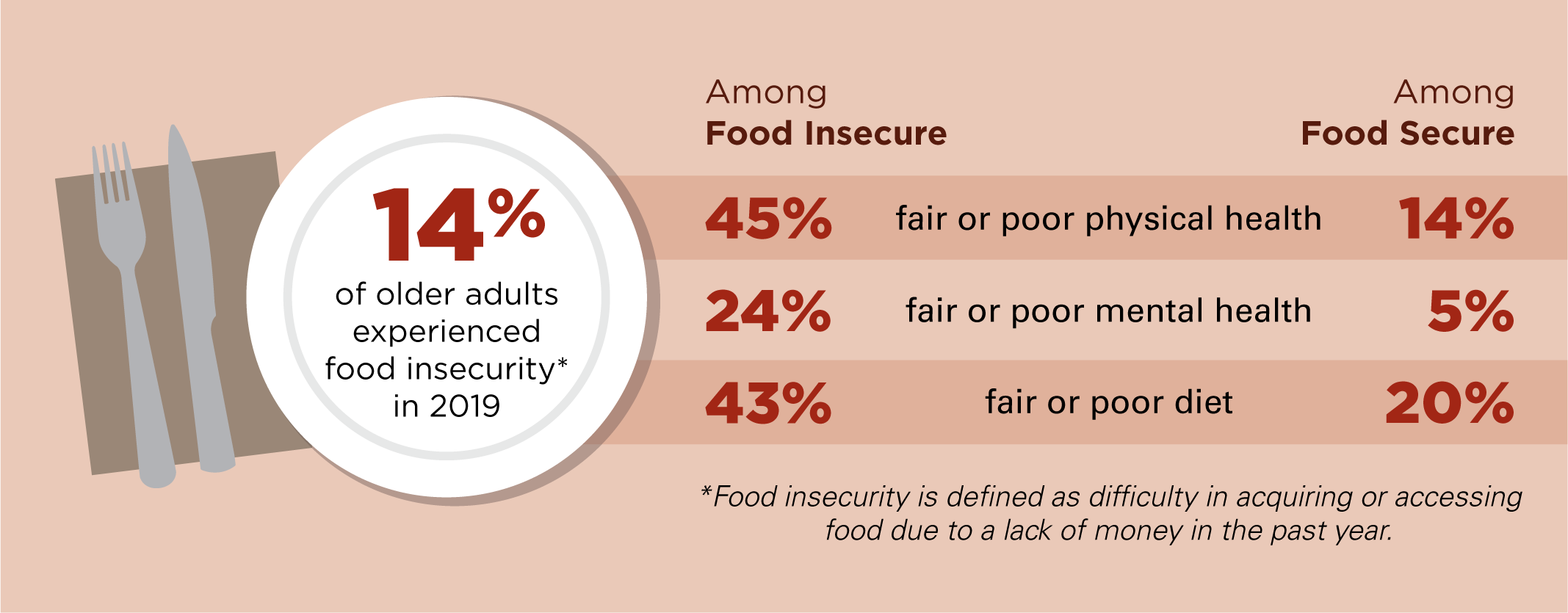
One in seven older adults (14%) in this survey reported experiencing household food insecurity in the past year. Common indicators of household food insecurity include not being able to afford balanced meals, eating less, skipping meals, or feeling hungry but not eating due to not having enough money for food. Among older adults who experienced household food insecurity in the past year, 42% reported severe food insecurity, meaning individuals in their household reduced the quality or quantity of foods they consumed due to limited resources.
Household food insecurity was higher among adults age 50–64 (17%) than adults age 65–80 (10%), and higher among non-Hispanic Black adults (22%) and Hispanic adults (22%) compared to non-Hispanic White adults (12%). It was also more common among older adults with a high school education or less (21%) compared to those with some college (13%) or a bachelor’s degree or higher (6%). Food insecurity was highest among those with annual household incomes less than $30,000 (32%), and higher among those with household incomes from $30,000 to less than $60,000 (20%) compared to those with household incomes of $60,000 or more (6%).
Food insecurity and health
Household food insecurity was associated with lower self-reported physical and mental health. Nearly half of adults age 50–80 who were food insecure rated their physical health as fair or poor (45%), compared to 14% of those who were food secure. Almost a quarter of those who were food insecure reported fair or poor mental health (24%) compared to 5% of those who were food secure. Furthermore, more than two in five older adults who were food insecure rated their diets as being fair or poor quality (43%) compared to 20% of those who were food secure.
Use of supplemental food and meal programs
During the past year, one in ten respondents age 50–80 (10%) reported receiving Supplemental Nutrition Assistance Program (SNAP) benefits (formerly known as food stamps), which provide a monthly supplement for purchasing nutritious food. One in three older adults experiencing food insecurity received SNAP benefits (32%) compared to 6% of older adults who were food secure. Receiving SNAP benefits was higher among non-Hispanic Black adults (21%) and Hispanic adults (15%) compared to non-Hispanic White adults (7%), and higher among adults with a high school education or less (17%) compared to adults with some college (9%) or a bachelor’s degree or higher (2%). Receiving SNAP benefits was highest among those with household incomes less than $30,000 (34%) compared to those with household incomes from $30,000 to less than $60,000 (8%) and incomes of $60,000 or more (3%).
Adults aged 60 and older are eligible to receive home-delivered or congregate meals (e.g. meals delivered in community or group settings) through the Older Americans Act (OAA). Yet among adults 60 and older, only 2% reported participating in meal programs through a community or senior center, and 1% received meals delivered to their home from a program like Meals on Wheels in the past year.
Implications
This poll found that one in seven adults age 50–80 experienced household food insecurity in the past year, with food insecurity more common among some subgroups of older adults. Household food insecurity was associated with lower self-reported physical and mental health and a lower perception of diet healthfulness among poll respondents.
Only 10% of older adults reported receiving SNAP benefits and very few received congregate or home-delivered meals. This suggests that some older adults experiencing food insecurity are not benefitting from programs designed to support them. Barriers to participating in SNAP or other community programs can include lack of knowledge or misinformation about services or eligibility, complex application procedures, waitlists, inadequate transportation, stigma, and other factors.
Improved communication about the benefits of participating in SNAP and community meal programs, as well as increased screening in clinical settings and referrals to community resources, may help to improve participation rates in nutrition programs and help alleviate food insecurity among older adults. These efforts are critically important as the COVID-19 pandemic has exacerbated existing financial and logistical challenges in accessing sufficient and healthy foods, making these programs essential for alleviating food insecurity, particularly among older adults.
Data and Methods
This National Poll on Healthy Aging report presents findings from a nationally representative household survey conducted exclusively by Ipsos Public Affairs, LLC (“Ipsos”), for the University of Michigan’s Institute for Healthcare Policy and Innovation. National Poll on Healthy Aging surveys are conducted using the Ipsos KnowledgePanel®, the largest national, probability-based panel in the U.S. Surveys are fielded two to three times a year with a sample of approximately 2,000 KnowledgePanel® members age 50–80.
This survey was administered online in December 2019 to a randomly selected, stratified group of older adults age 50–80 (n=2,048). Respondents were selected from the Ipsos web-enabled KnowledgePanel®, which closely resembles the U.S. population. The sample was subsequently weighted to reflect population figures from the U.S. Census Bureau.
The completion rate was 77% among panel members contacted to participate. The margin of error is ±1 to 2 percentage points for questions asked of the full sample, and higher among subgroups.
Findings from the National Poll on Healthy Aging do not represent the opinions of the University of Michigan. The University of Michigan reserves all rights over this material.
Read other National Poll on Healthy Aging reports and about the poll's Michigan findings, and learn about the poll methodology.
Citation
Leung C, Malani, P, Singer D, Kirch M, Solway E, Kullgren J, Wolfson J. How Food Insecurity Affects Older Adults. University of Michigan National Poll on Healthy Aging. May 2020. Available at: http://hdl.handle.net/2027.42/155333
Scholarly Publications
Leung CW, Kullgren JT, Malani P, et al. Food insecurity is associated with multiple chronic conditions and physical health status among older US adults. Prev. Med. Rep. 2020. https://doi.org/10.1016/j.pmedr.2020.101211
Wolfson JA, Leung CW, Kullgren JT. Food as a critical social determinant of health among older adults during the Coronavirus Disease 2019 (COVID-19) pandemic. JAMA Health Forum. July 31, 2020;1(7):e200925. doi:10.1001/jamahealthforum.2020.0925