
As COVID-19 began to spread across the U.S. in early 2020, health systems made rapid and sweeping changes to how care was delivered. These changes sought to help slow the spread of COVID-19 by keeping as many people home as possible. This shift led many patients, including many older adults, to have appointments with their health care providers through telehealth visits (typically conducted by video or phone) rather than in-person.
In June 2020, the University of Michigan National Poll on Healthy Aging (NPHA) surveyed a national sample of U.S. adults age 50–80 about their experiences related to telehealth visits; this was a follow-up to a similar NPHA survey conducted with a different national sample in May 2019. These surveys offer a unique opportunity to see how much has changed over the past year, which saw COVID-19 disrupt daily life in an unprecedented way.
Changes in telehealth visits
From 2019 to 2020, there was a substantial increase in the proportion of older adults who reported that their health care providers offered telehealth visits. In May 2019, 14% of older adults said that their health care providers offered telehealth visits, compared to 62% in June 2020.
Similarly, the percentage of older adults who had ever participated in a telehealth visit rose sharply from 4% in May 2019 to 30% in June 2020. Of those surveyed in 2020, 6% reported having a telehealth visit prior to March 2020, while 26% reported having a telehealth visit in the period from March to June 2020.
Among adults age 50–80 who had a telehealth visit in the period from March to June 2020, 76% reported it was with a primary care provider, 32% with a specialty care provider, and 18% with a mental health provider. Respondents said that their most recent telehealth visit was conducted via video by phone (33%), video by tablet or computer (31%), or by phone with audio only (36%).
In June 2020, 30% of older adults with a telehealth visit said that video or phone visits were the only options available when scheduling their appointment. Nearly half (46%) indicated that in-person visits were canceled or rescheduled to telehealth visits by their health care provider. Fewer than one in six (15%) reported that fear of COVID-19 led them to request or reschedule an in-person appointment as a telehealth visit.

Telehealth versus in-person office visits
When adults age 50–80 who had ever had a telehealth visit compared office visits to telehealth visits, the majority perceived office visits as providing a higher overall quality of care (58% in May 2019 vs. 56% in June 2020) and better communication with health care providers (55% in May 2019 vs. 54% in June 2020). However, in both surveys, telehealth visits were perceived as more convenient than office visits (47% in May 2019 vs. 56% in June 2020). In the past year, a greater proportion of older adults reported that the amount of time spent with the health care provider was about the same during telehealth and office visits (31% in May 2019 vs. 42% in June 2020).
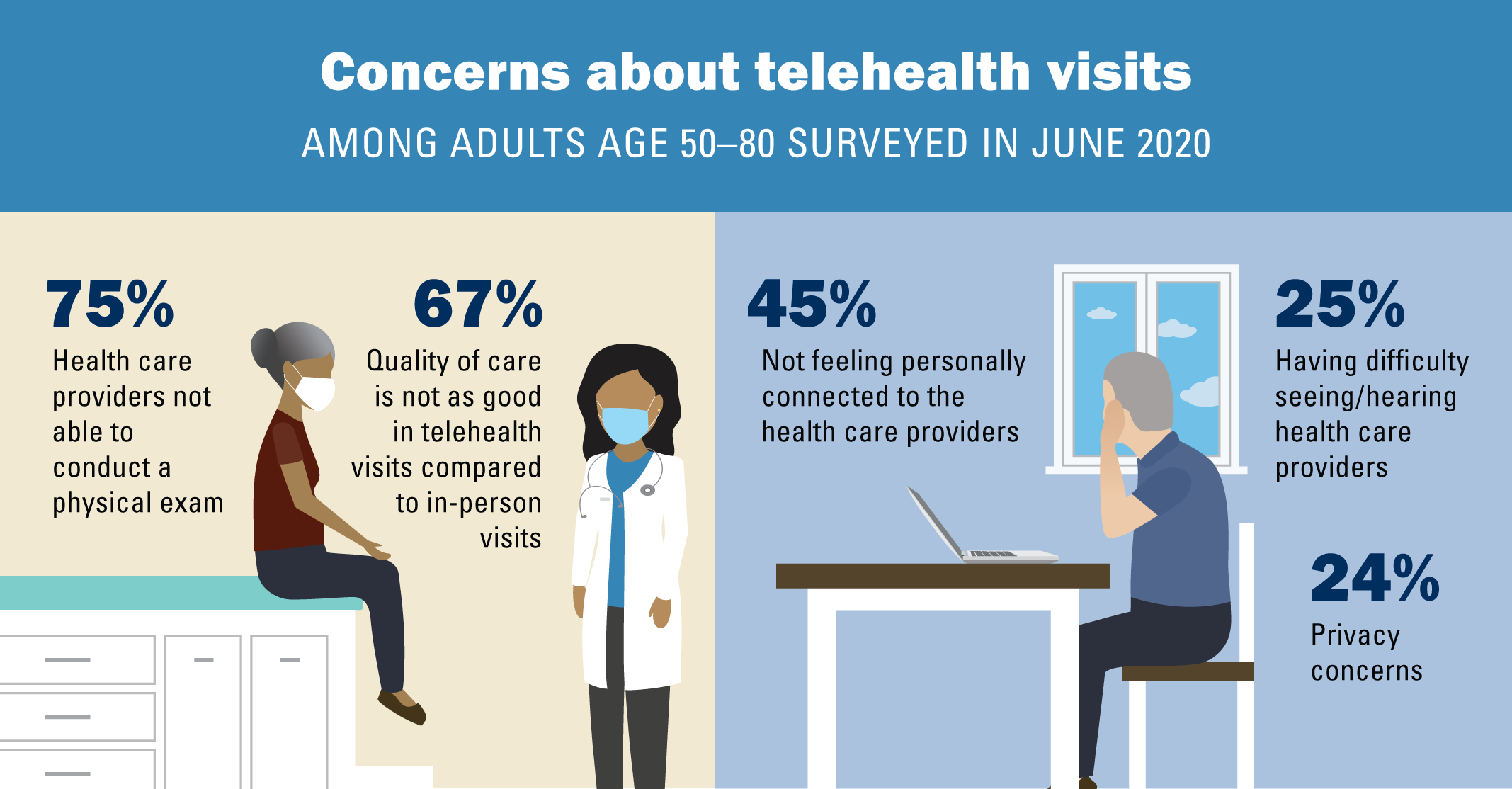
Concerns about telehealth visits
The most common concerns about telehealth visits among older adults surveyed in June 2020 were that a health care provider cannot conduct a physical exam (75%) and that the quality of the care is not as good as in-person (67%). Other concerns noted were not feeling personally connected to the health care provider (45%), having difficulty hearing or seeing the health care provider (25%), and privacy (24%).
Over the past year, some concerns about telehealth visits decreased among adults age 50–80 whether or not they had a telehealth visit. Older adults’ concerns about privacy in telehealth visits decreased from 49% in May 2019 to 24% in June 2020, and concerns about having difficulty seeing or hearing health care providers in telehealth visits decreased from 39% in May 2019 to 25% in June 2020. Concerns about not feeling personally connected to the health care provider decreased slightly (49% to 45%).
In the June 2020 survey, those who had a telehealth visit were less likely than those who did not have a telehealth visit to report concerns with privacy, difficulty seeing or hearing the health care provider, and/or not feeling personally connected to the health care provider (see supplemental data table).
Comfort with video technology
The proportion of older adults who said that they were comfortable with video conferencing technologies (e.g., FaceTime, Skype, or Google Hangout) rose from 53% in May 2019 to 64% in June 2020. Additionally, in June 2020, fewer people reported that they have never used these technologies compared to May 2019 (17% vs. 28%). Those who had reported ever having a telehealth visit in the June 2020 survey were more likely than those who did not to be comfortable with video technologies (74% vs. 60%). The majority (91%) found it easy (64% very easy, 27% somewhat easy) to use the technology necessary to complete their telehealth visit, and 9% found it somewhat or very difficult.
Interest in future telehealth visits
In both surveys, older adults were presented with hypothetical scenarios to gauge their interest in future telehealth visits based on the reason for the visits. For a one-time follow-up visit after a medical procedure or surgery, interest in a telehealth visit rose from 55% in May 2019 to 63% in June 2020. For a visit with a provider whom they had previously seen, interest in a telehealth visit rose from 58% in May 2019 to 72% in June 2020. For a new patient visit or to discuss a new health problem, interest in a telehealth visit was similar in May 2019 (34%) and June 2020 (36%).
In June 2020, those who had a past telehealth visit were also more likely than those who never had one to be interested in future telehealth visits with a primary care provider (70% vs. 55%), a specialty care provider (58% vs. 45%), or a mental health provider (41% vs. 28%).
Among older adults who expressed interest in future telehealth visits in 2020, 45% said they were more interested in telehealth because of COVID-19, 50% had the same level of interest, and 5% were less interested. Those who had a past telehealth visit were more likely than those who never had a telehealth visit to be more interested in a future telehealth visit (51% vs. 41%).
Implications
COVID-19 has led to dramatic changes in nearly all facets of life. Within the U.S. health care system, one of the most substantial shifts has been the rapid expansion of telehealth services. These changes are likely to remain long after the COVID-19 pandemic subsides. Given that the COVID-19 pandemic will persist for some time, and older individuals will remain at higher risk of its harmful effects, telehealth utilization is expected to continue to increase and become a standard part of health care services for older adults.
Results from this 2020 National Poll on Healthy Aging show that older adults have experienced the rapid expansion of telehealth visits. Availability, use, and interest all increased substantially over one year, as did the personal use of and comfort with video conferencing technologies commonly used in telehealth visits. As more people have experienced telehealth visits in the past year, some perceived concerns, including privacy and communication with health care providers, have diminished. Among those who have had telehealth visits, there were upward changes in perceptions in the overall convenience of telehealth visits.
While the vast majority of older adults who had a telehealth visit reported that the technology was easy to use, some older adults have limited experience and comfort with technology and may need additional support. Furthermore, some older adults continue to express concerns about telehealth visits, particularly
regarding the quality of care compared to in-person visits and not being able to get a physical exam. Until these issues are addressed, some older adults may be hesitant to engage in telehealth visits.
Telehealth is already becoming and is likely to remain an important part of health care delivery. Continued tracking of its usage among older adults and their experiences is essential to inform best practices and optimize use.
Data Source and Methods
This National Poll on Healthy Aging report presents findings from a nationally representative household survey conducted exclusively by Ipsos Public Affairs, LLC (“Ipsos”) for the University of Michigan’s Institute for Healthcare Policy and Innovation. National Poll on Healthy Aging surveys are conducted by recruiting from Ipsos KnowledgePanel®, the largest national, probability-based panel in the U.S.
This survey module was administered online in June 2020 to a randomly selected, stratified group of older adults age 50–80 (n=2,074). The sample was subsequently weighted to reflect population figures from the U.S. Census Bureau.
The completion rate was 78% among panel members contacted to participate. The margin of error is ±1 to 2 percentage points for questions asked of the full sample and higher among subgroups.
Findings from the National Poll on Healthy Aging do not represent the opinions of the University of Michigan. The University of Michigan reserves all rights over this material.
Read other National Poll on Healthy Aging reports and about the poll's Michigan findings, and learn about the poll methodology.
Citation
Buis L, Singer D, Solway E, Kirch M, Kullgren J, Malani P. Telehealth Use Among Older Adults Before and During COVID-19. University of Michigan National Poll on Healthy Aging. August 2020. Available at: http://hdl.handle.net/2027.42/156253